

Copyright © 2004, Mary Carten/Vita Gagne
With
love and gratitude, this booklet is dedicated to the memory of
Dr.
Steven E. Kopits, friend and healer of diastrophics and all little people,
and to ALL doctors who strive for answers in their care of little people.
| DIASTROPHIC
DYSPLASIA by Mary Carten and Vita Gagne
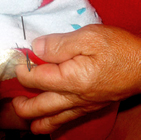
A diastrophic baby may be born with, or develop, the following characteristics:
Despite these limitations, DD children learn to improvise when it comes to their hands. No surgical invention is warranted or needed. If given the opportunity, most DDs are capable of even the most complex manipulation tasks. |
 |
 |
 |
 |
 |
 |
 |
 |
|
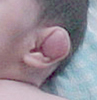
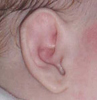
THOSE CAULIFLOWER EARS
|
 |
 |
 |
 |
|
Typical
ear swelling
|
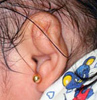
Resolution
of
same ear |
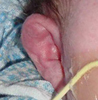
Typical
ear
swelling #2 |
Ear
#2 after compression method
|
|
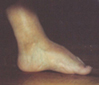
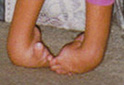
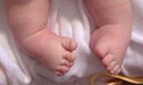
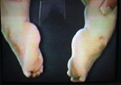
DIASTROPHIC CLUBFEET - UNIQUE AND COMPLEX Diastrophic children are usually born with clubfoot deformities, having more components than a clubfoot in an average-sized child. These deformities may range from very mild to severe. Operations to correct this problem are usually done at age 1-2 years, and may include release of the heel tendon and often more involved procedures to correct the other components of the DD clubfoot. The great toe often presents in a "hitchhiker" position requiring correction. Many of these children and adults require custom-made shoes to accommodate their wide feet. |
 |
 |
 |
|
Mild
DD foot
|
Severe
DD feet
|
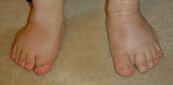
Typical
DD infant feet
|
 |
 |
 |
|
Rear
view of feet
before correction |
Same
feet
after correction |
Regular
shoe
with added strap |
 |
 |
 |
|
Custom
made shoes
|
Pedorthist
adapted
athletic shoes |
Pedorthist
adapted
dress shoes |
|
CERVICAL AND SPINAL CHANGES
- Head control,
2.5 months
|
 |
 |
 |
|
Biking
|
Swimming
Therapy
|
Physical
Therapy
|
|
An adult diastrophic usually walks with a forward tilt appearing to be falling forward. This is caused by a number of factors, such as deteriorating hips and knees as well as progressive spinal curvatures. Weight gain may also be a factor as many adults must rely on a motorized scooter for mobility. Hip and knee replacements are helping many adults regain some of their lost mobility. Some adults are fortunate enough to be able to continue using walkers and canes.
The administration of anesthesia to a diastrophic dwarf should be closely monitored. It is very important that prior to any surgery that all diastrophics have x-rays of their cervical spine to determine if they have abnormalities, particularly kyphosis or abnormal motion. The placement of the endotracheal tube for breathing during general anesthesia typically requires the neck be hyperextended for the insertion. This can be dangerous if the cervical spine has kyphosis or abnormal motion since compression of the spinal cord and or nerve roots could occur, leading to paralysis. Infants and children sometimes have very small tracheas and require special skill in tube placement.
Pregnancy for adult DD females can and does happen. A DD female generally will have an average-sized baby, unless her partner is also a dwarf, and sometimes even then the baby will be average-sized. Consultation with a genetic dwarfism specialist before pregnancy occurs is suggested.
Serial ultrasounds should be done to monitor the baby's growth and position. All deliveries are done by caesarean section and are usually planned to take place within 2-4 weeks of actual due date. This is a major complication even if it is planned. Tests are done of the baby's lungs to ensure full development. General anesthesia is used most often, although there have been reports of success with an epidural. In some cases, the baby must remain in the hospital a few extra days to gain those extra ounces before being released. Recovery for the new DD mom should be a speedy and enjoyable time of getting to know her new little treasure. |
 |
 |
|
Mother
and Daughter (age 1)
|
Mother
and Daughter (adult)
|
|
Fathers
can be Diastrophic too! |
|
 |
 |
|
Diastrophic
Siblings |
|
|
|
|
 |
 |
RESOURCES
Little People
of America, Inc.
1-888-LPA-2001
Little People of America (LPA) Online: http://lpaonline.org/
Diastrophic
Help website: http://pixelscapes.com/ddhelp/
Online Medical Dictionary: http://www.nlm.nih.gov/medlineplus/mplusdictionary.html
National Organization for Rare Disorders, Inc.:
http://hw.healthdialog.com/kbase/nord/nord482.htm
ACKNOWLEDGMENTS
The author wishes to thank Dr. Charles Scott and Dr. Cheryl Reid for their help as a medical resource, Dr. Monica Carten for her review of the booklet, and Vita Gagne for her editing and graphics talents and the preparation of this booklet.
REFERENCES
This
document and all of its contents are copyright © 2004 by Mary Carten and
Vita Gagne. In addition, all photographs in this document are the copyrighted
property of the authors or the individuals pictured, and are used with their
permission. All rights reserved. To obtain legal copies of these photographs
for any purpose whatsoever, contact Vita Gagne.
This booklet is
also available in PDF format: http://pixelscapes.com/ddhelp/Diastrophic-Dysplasia.pdf
![]() Main
Page
Main
Page